Autonomic Nervous System Testing
Autonomic nervous system testing is used to assess whether the autonomic nervous system (ANS) is functioning normally. The ANS is responsible for controlling automatic body functions, such as blood pressure, body temperature, digestion, and breathing.
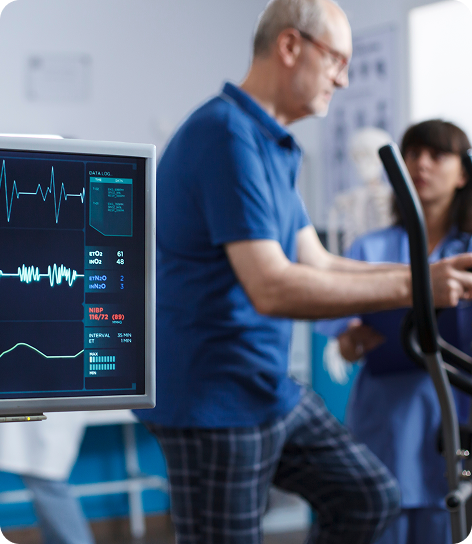
Any issue with the ANS is called autonomic dysautonomia. Autonomic dysfunction may result from diabetic autonomic neuropathy, heart disease, some medications, autoimmune conditions, head trauma, neuropathy, and certain infections. It can also manifest as pure autonomic failure.

Who Needs Autonomic Nervous System Testing?
Autonomic nervous system testing is recommended for patients who experience dizziness, fainting spells, sweating abnormalities, rapid heartbeat, or temperature instabilities. These are common symptoms of autonomic disorders.
Types of Autonomic Nervous System Testing
Autonomic testing consists of several specialized evaluations, such as:
Tilt Table Test
This test evaluates how your autonomic nerves regulate blood pressure and heart rate when changing positions from lying down to standing. It is particularly useful for diagnosing autonomic dysfunction and orthostatic hypotension.
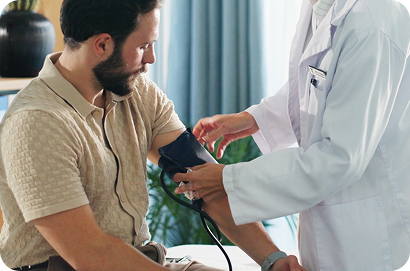
Valsalva Maneuver with Deep Breathing
Measures heart rate and blood pressure changes during deep breathing. Electrodes on the chest monitor heart rate, while a cuff measures blood pressure. This test helps evaluate autonomic function testing and autonomic response testing.

Quantitative Sudomotor Axon Reflex Test (QSART)
Assesses the small autonomic nerves that control sweating. Electrodes are placed on the skin, often on the foot, leg, and wrist, to measure how the sweat glands and nerves respond to mild electrical stimulation. This test is part of the autonomic reflex screen protocols to evaluate the autonomic nervous system function.

Frequently Asked Questions
What symptoms suggest I might need autonomic nervous system testing?
Symptoms include dizziness, fainting, abnormal sweating, rapid heart rate, temperature instability, and blood pressure problems.
What conditions can ANS testing help diagnose?
Testing helps identify autonomic dysfunction linked to diabetic neuropathy, autoimmune disease, heart disease, nerve damage, infections, and other autonomic disorders.
What does the tilt table test feel like, and is it uncomfortable?
You are secured to a table that moves from lying to upright. Some people feel lightheaded or dizzy briefly, but the test is closely monitored for safety.
How long does the full autonomic testing process take?
The full evaluation typically takes 30 minutes to 1 hour, depending on the number of tests performed.
Do I need to stop any medications before the test?
Some medications, caffeine, and nicotine may need to be avoided beforehand to ensure accurate results. Instructions vary by test and your physician will advise you accordingly.
Are ANS tests safe for people with heart conditions or fainting episodes?
Yes. Testing is performed under medical supervision and is designed to safely assess patients who already experience fainting or blood-pressure issues.
What happens if my results show autonomic dysfunction?
Your neurologist will explain the findings and create a care plan to manage symptoms, address possible underlying causes, and improve autonomic regulation.
Will I be able to drive or return to normal activities after the tests?
Most patients can resume normal activities the same day, although some may need short rest if dizziness occurs during testing.
Is autonomic nervous system dysfunction treatable?
While not always curable, autonomic dysfunction is manageable with targeted treatment, lifestyle adjustments,
How soon will I receive my test results and a care plan?
Results are typically reviewed shortly after testing, followed by discussion of findings and next steps with your provider.
When to Reach Out
If you or a loved one in Westchester or NYC is experiencing symptoms of autonomic disorders or autonomic dysfunction, scheduling a consultation with our neurologist is recommended. Our team can provide comprehensive autonomic testing and guide appropriate care.
Call us today at (914) 816-1941 or email info@chesterneurology.com to schedule an appointment.
We serve families in Westchester, the Bronx, Manhattan, and more, all with compassion, clarity, and commitment.
Take the First Step
Contact Us Today
Early diagnosis and correct identification makes planning, treatment, and care accessible to everyone.
